PROPRIOCEPTION: YOUR SIXTH SENSE
Why movement and sensation are inextricably linked
By: Elise Walker
Have you ever tried drinking out of a straw after a mouth-numbing trip to the dentist? Hilarity can ensue. Or maybe you have slept in an awkward position and awoken with a dead arm, which you then flail about in order to revive? (Occasionally to the detriment of your bedside water glass.) For most of us, these incidents are but brief annoyances. Yet, they illustrate a powerful connection between sensation and movement that is hard to appreciate until it is lost.
To better understand how sensation and movement are linked, let’s take a closer look at the phenomena of a dead limb. This issue stems from a problem in your nerves. Normally, nerves running throughout your entire body are the pathways for rapid communication to and from your brain. These pathways are made up of motor nerves, which send command signals down from the brain, and sensory nerves, which carry sensation messages back to the brain. When you fall asleep on your arm, pressure on your nerves and their blood supply can essentially choke off the flow of the messages – like a kink in a garden hose.
Sensory nerves are usually affected first, but motor nerves can also be cut off if you’re really zonked out. As a result, when you finally wake up, you can’t feel your arm and sometimes you can’t even move it. As the effect starts to wear off, your motor nerves quickly come back online and then your sensory nerves follow (with the characteristic sensation of burning or tingling as things get back to normal). However, before sensation returns, there is a period of time when you can move your arm but not feel it – and this is when your attempt to reach for that drink of water results in a crazy left hook.
So, why is sensation so crucial for fluid, precise movement? A large part of this is due to the structure and function of our muscles.
 The human body has many types of muscles, but the most abundant are the skeletal muscles, which wrap around the framework of your skeleton. Skeletal muscles are voluntary muscles, meaning we can directly control them with our brains. From the explosive pitch of a baseball to the delicate manipulation of a paintbrush, these muscles are powerful and precise. But, many people don’t realize that muscles are also important sensors.
The human body has many types of muscles, but the most abundant are the skeletal muscles, which wrap around the framework of your skeleton. Skeletal muscles are voluntary muscles, meaning we can directly control them with our brains. From the explosive pitch of a baseball to the delicate manipulation of a paintbrush, these muscles are powerful and precise. But, many people don’t realize that muscles are also important sensors.
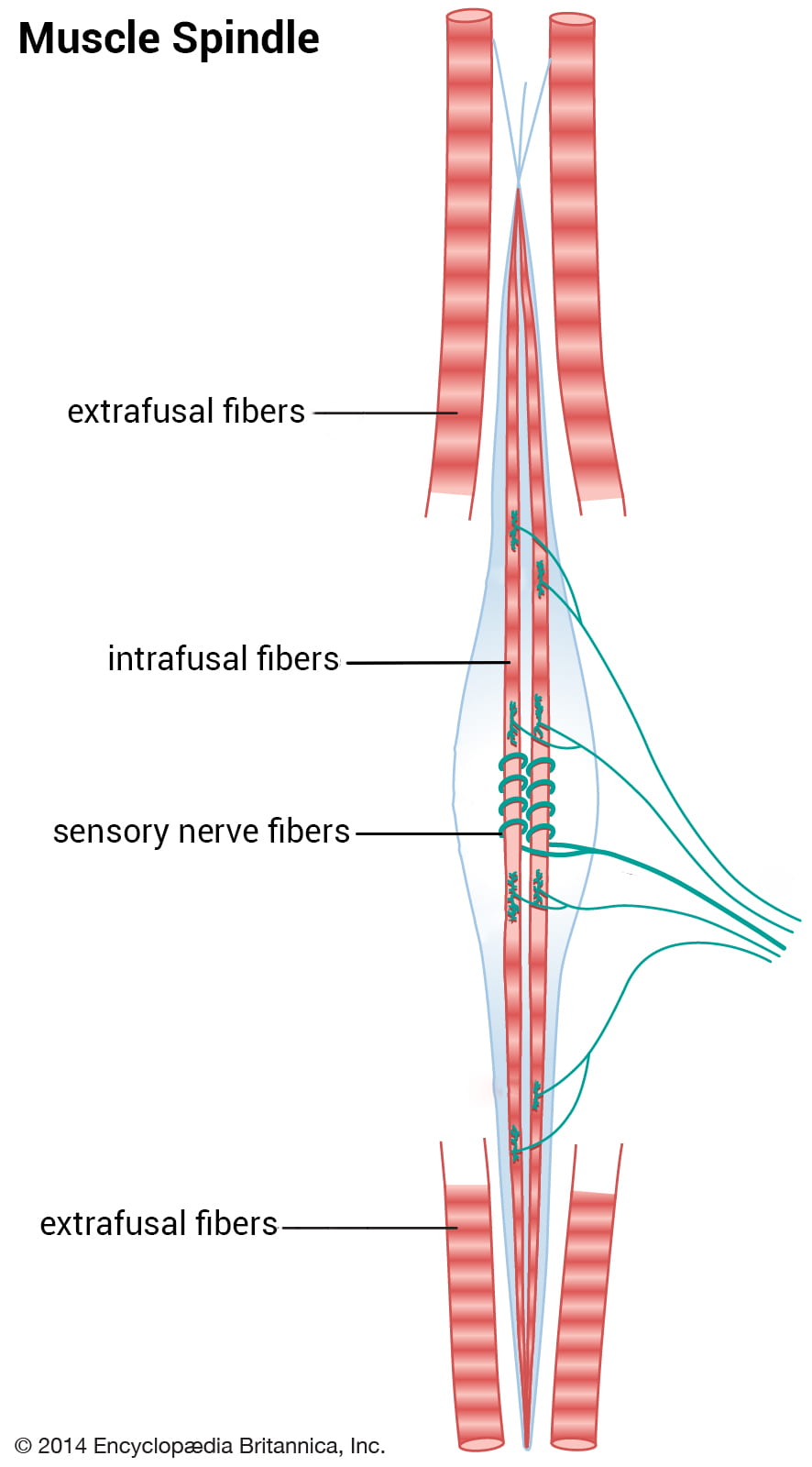
A muscle is essentially a big bundle of fibers of varying size and function. Large fibers on the outside do the brunt of the work, contracting powerfully to pull on different parts of the skeleton and create movement. Within these larger fibers are sensory fibers called muscle spindles, which move along with the outer fibers. Muscle spindles are specialized for sensation because they have sensory nerve fibers wound tightly around them like little springs. These springs stretch rather than pull, sending messages up to the brain to communicate how fast a muscle is moving.
Your brain receives signals from all your muscle spindles, along with other sensory receptors in your tendons and joints, and constructs an overall sense of the position and motion of your body. Hence, even with your eyes closed you can touch your nose, wave your hand, or toss a ball, remaining confident in where your arm is. This remarkable ability is called proprioception, and it is sometimes called the “sixth sense” (after sight, smell, taste, touch and hearing).
Proprioception is a sense that we often overlook because it is only subtly distinguished from movement. And, unlike sight or hearing or taste, we rarely experience the absence of proprioception (dead arm being a rare exception). Yet, a total loss of proprioception might be even more devastating than going blind or deaf. Without sensory information coming in from our muscles, we would be unable to monitor and correct our paths of motion. Imagine trying to walk, gesture, or eat if you had no sense of where your limbs were without looking at them.
Few people can understand the burden of proprioceptive loss better than an amputee. When a limb is lost, the ability to move and sense are both gone. The first thing that must be restored is the limb itself, and recent advances in prosthetic design have resulted in some pretty cool powered limbs that can closely mimic natural movement.
However, studies show that a surprising number of amputees end up leaving the fancy new equipment in the closet, opting for a simpler prosthetic or none at all. One major reason for this is the lack of sensory capabilities, especially in the realm of proprioception. Without sensory feedback, even the most dexterous prosthetic arm is severely limited. A task that should be easy, like picking up a glass of milk, requires great concentration and constant visual guidance.
That is why one of the newest initiatives in government-funded research is called HAPTIX (Hand Proprioception and Touch Interfaces). HAPTIX hopes to bridge the gap between movement and sensation in prosthetic arms. Using external sensors to sense pressure, movement, or texture, HAPTIX aims to create a safe and reliable interface by connecting sensors to the nerves that are left above the point of amputation.
For instance, in one new study, researchers implanted tiny cuff electrodes around the three main nerves of the forearm. Because cuff electrodes wrap around the outside of a nerve, they do less damage than electrodes that pierce the nerve, ensuring longevity. Through multiple channels on each electrode, electrical impulses can be applied with varying intensity and frequency. In the lab, implanted amputees were wired up to a computer so that the researchers could experiment with different stimulation patterns. In doing so, they were able to create sensations like tingling, pressure, and texture. Importantly, amputees showed a dramatic improvement with delicate tasks when they were wired in to feedback from sensors on the prosthetic finger.
There is still much to do before the goal of HAPTIX is truly achieved. Wireless electrodes will allow for an untethered prosthesis, and refined nerve stimulation is needed to achieve precise sensations, such as those required for proprioception. But sensitive prosthetics offer benefits beyond improved control. For instance, phantom pain is a common complaint of amputees: painful sensations that seem to come from the missing limb. Remarkably, phantom pains seem to subside if you give the sensory nerves something to do.
Proprioception and touch should also restore “embodiment,” helping amputees to view their prosthetic as a true extension of their body rather than just a fancy tool. This sheds light on an important role of proprioception for all of us. It seems that sensation, and muscle sense in particular, is crucial for a healthy metaphysical self-image. In the experience of one patient, a senseless arm is viewed as a completely alien entity. In another rare case of complete sensory loss, bedtime was distressing because closing his eyes left the patient feeling unembodied, floating.
It seems that Descartes’ principle could be rephrased as “I sense, therefore I am.” Hopefully HAPTIX researchers will be able to restore this sensory awareness to amputees soon, and to others suffering from sensory loss. In the meanwhile, the next time your arm falls asleep, pause and consider: Do you feel less you?

